Infants who are born via assisted reproductive techniques, like IVF, go through additional growth and development phases during the laboratory embryonic stage. Before the embryos are placed in the mother's uterus, the embryologists grade them using several techniques. Examining the embryo's quality grade in a lab to choose a better-quality one for transferring is one of the crucial steps in the IVF process.
One of the key elements of a successful IVF procedure is the grading system of the embryos. During an IVF procedure, embryologists use a tool called embryo grading to assist them choose precisely which embryos to transfer, the best day for the transfer, and the right quantity of embryos to transfer. Since the embryo is often implanted into the uterus on day 3 (cleaving stage) or 5 (blastocyst stage), it is critical to look at certain embryo traits, such as the Inner Cell Mass (ICM), Trophectoderm (the placenta's cell layer, as well as the membranes that enclose the embryo), and the degree of blastocyst expansion, to identify a viable embryo.
It is also important to note that embryo grading is not utilized alone. The patient's age, fertility history, and other details should also be taken into account when selecting the most viable embryos.
Why Embryo Grading is Essential in IVF
A patient's embryos' quality can be evaluated by embryologists and doctors so they can choose which embryos to transfer first. A favorable outcome (live birth) is more likely for a good quality embryo than a poor quality embryo, but the grade by itself does not guarantee this.
It's critical to keep in mind that hand morphological grading is arbitrary. Scoring can differ depending on the lab and embryologist. To distinguish between embryos that are aneuploid (chromosomally defective) and euploid (chromosomally normal), many labs today perform PGT-A in addition to embryo grading (chromosomally abnormal). Prioritizing the transfer of euploid embryos with the best morphological grade is the standard of treatment for such clinics.
Finally, embryo grading is a helpful tool that your doctors can utilize to increase the likelihood that your IVF cycle will be successful at the time of transfer.
Criteria Used in Examining Embryo Characteristics
The following criteria and terminology are used by embryologists to describe the properties of the embryos.
Morphology
The shape and organization of an embryo are referred to as its morphology. Experts frequently refer to the evaluation of morphology as the examination of embryo traits.
Morula
The cells enter the blastocyst-forming stage, where they are unable to be separated from one another, a few days after fertilization, after the embryo has gone through numerous cell types or division phases. A morula, also known as this stage, normally appears between days 3 and 4 following fertilization.
Blastocyst
After 5 to 6 days following fertilization and cell division, the embryo enters the blastocyst stage. A blastocyst is a stage in the embryo development during which the blastocoel cavity, trophectoderm (surface cells), and inner cell mass are created.
Inner Cell Mass (ICM)
The blastocyst's Inner Cell Mass (ICM) is a collection of cells that will eventually develop into the fetus. The cells that surround the blastocyst's outer layer, or trophectoderm, play a role in embryo implantation. The placenta eventually develops from these cells.
Determining Embryo Quality in IVF
The embryo's quality is often assessed on day 3 or day 5 following egg retrieval and laboratory fertilization. For this reason, the majority of the embryo's growth and development occur within the egg until day 3. The sperm genetic material begins to enter the embryo's DNA by the end of day three, at which point the embryo's genetic makeup is complete and functional. On day 5, the blastocyst growth, trophectoderm, and inner cell mass are measured to grade the embryo.
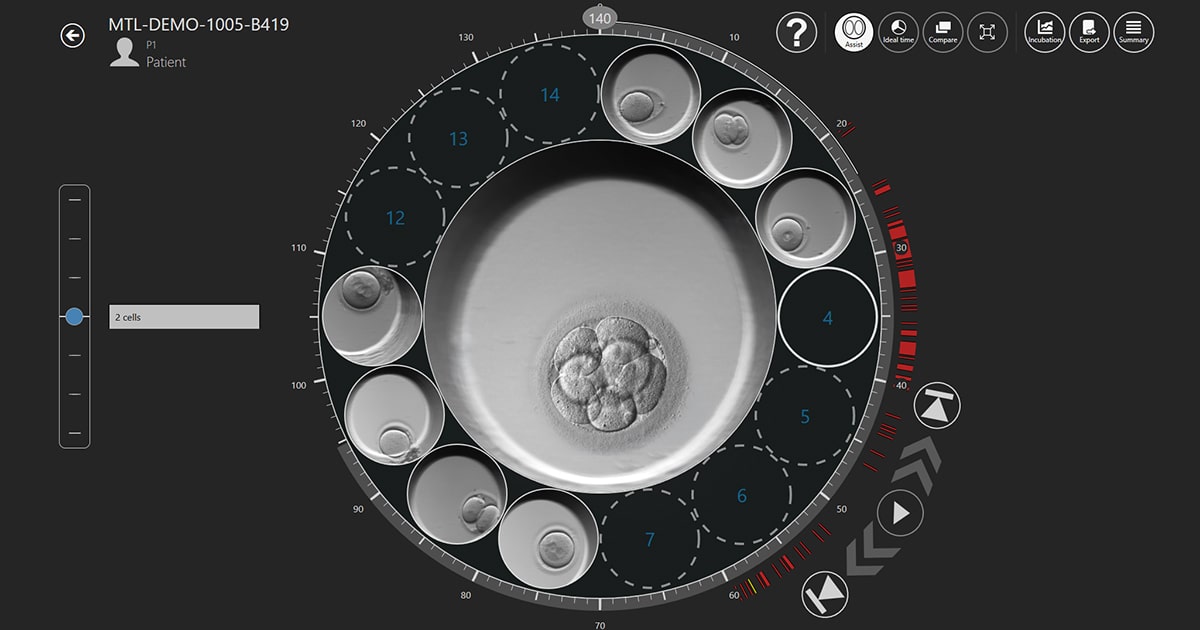
Grading Day 3 Embryos (Cleavage Stage Embryos)
Day 3 Embryos (D3) are known as cleavage stage embryos. This indicates that while they are cleaving or dividing, the embryo itself is not expanding in size. They normally consist of 6–8 cells enclosed in a shell-like outer layer known as the zona pellucida. At this stage of development, embryos are graded on rate of growth and degree of fragmentation, and they can be graded into three:
Grade A
These embryos have little or minimal cell fragmentation, 6–8 uniformly sized cells, and no more than 10%.
Grade B
These embryos have a number of cells that are 25–50% fragmented and have more uneven or irregular shapes.
Grade C
These embryos have fragmentation of at least 50% and consists of uneven cells.
Grading Day 5 Embryos (Blastocysts)
Grading on Day 5 (D5) Embryos, also known as a blastocyst, is more common since most clinics employ the Gardner and Schoolcraft three-part scoring system. During the blastocyst development stage, embryos should begin to expand past the zona pellucida, or shell, by day 5.
There are three ways to score blastocycts: degree of expansion (depending on how wide the cavity is), appearance of the Inner Cell Mass (ICM), which is graded for cell compaction, and trophectoderm appearance. These elements can also be ranked from A to C, with A being the best.
Blastocyst Grading System
Rating blastocysts follows a three-part system (as mentioned above), consisting a number and two letters.
The number indicates the degree of the expansion of the embryo’s cavity, ranging from 1-6. The blastocyst expansion degree refers to how much the blastocyst expands. The blastocoel, an embryonic chamber filled with fluid, is measured at this stage and ranges in size from 1 to 6. At this point, size 6 is ideal.
Number 1 - The blastocoel cavity has filled less than half of the embryo.
Number 2 - The blastocoel cavity fills a third of the embryo.
Number 3 - The blastocoel cavity has partial expansion and fills 70% of the embryo.
Number 4 - Fully expanded blastocoel cavity cavity.
Number 5 - embryo has expanded and split open the zona.
Number 6 - embryo has completely hatched from the zona.
The first letter and grade indicates the Inner Cell Mass (ICM) quality.
Grade A - Clump of cells are well-defined, tightly packed, and embryo cells are uniform.
Grade B - Clump of cells are less well-defined may appear grainy. Less homogeneous embryonic cells have some small fragmentation.
Grade C - Cells are dark and appear degenerative.
Finally, the second letter and grade indicates the trophectoderm quality. The process of creating the placenta and other prenatal tissues determines the trophectoderm quality.
A - The trophectoderm show many smooth cells with equal sizes forming a neat layer.
B - The trophectoderm shows an irregular cell layer with some grainy cells.
C - The trophectoderm shows a very irregular cell layer, and cells may be dark and grainy.
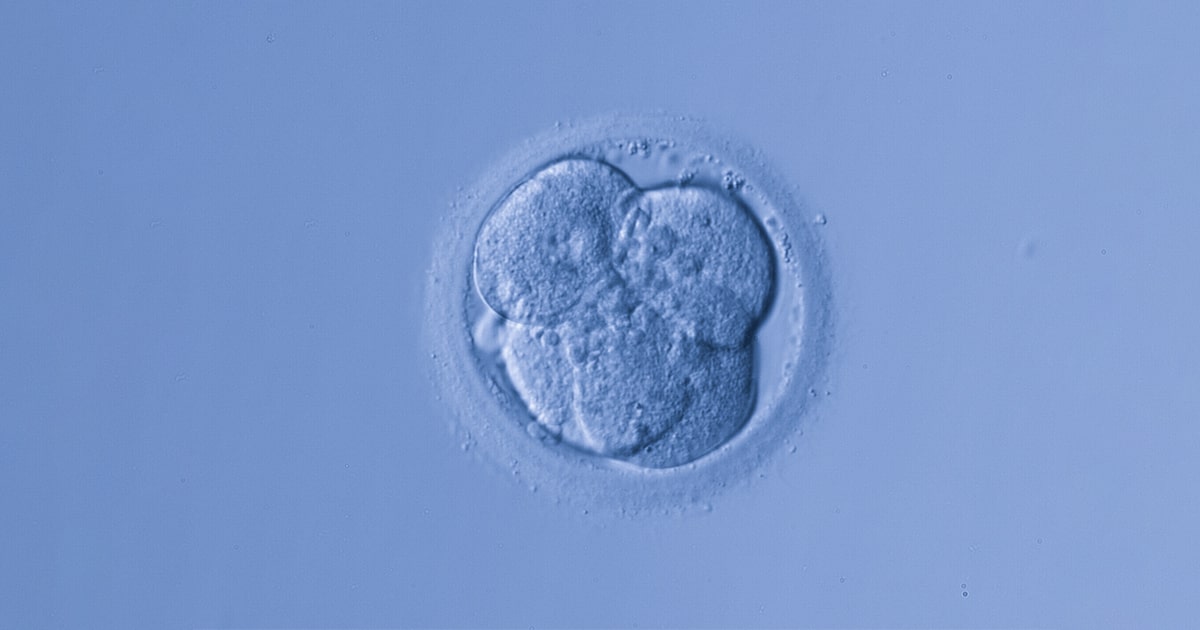
IVF Success Rates Using Embryo Grading
During a five-year period, a study at a Canadian fertility clinic examined the live birth rate for patients who underwent fresh or frozen embryo transfers. The grades for inner cell mass (ICM) and trophectoderm epithelium (TE) revealed that the live birth rates for AA grade embryos were 41.4%, BB grade embryos were 31.3%, and CC grade embryos were 13.3%. They discovered that while CC embryos might still result in pregnancy, the chances were far lower than for AA or BB embryos.
Esco Medical
Embryo grading is a great tool used by fertility centers, but it is only one of the important steps in the embryo selection process. Because of this, our embryologists and scientists take into account a lot of factors, such as the entire medical history of a patient and other genetic testings, in addition to the embryo grade when determining an embryo's potential.
Giving our patients the best possibility of a successful pregnancy is our main priority at Esco Medical. Learn more about IVF products here.








