The worldwide in vitro fertilization (IVF) services have been projected to show significant growth due to an increase in infertility rate, an inclination of delayed pregnancies, and the rise in IVF success rate. With this, expansion in fertility tourism paved way for the growth in the number of fertility clinics and a more aggressive campaign about fertility education. It is believed that fertility needs to be talked about as part of gender fairness and social equality concerns in both education and healthcare.
Table of Contents:
What is In Vitro Fertilization (IVF)?
In Vitro Fertilization (IVF) is a form of fertility treatment done in a laboratory wherein the sperm cells are placed together with an unfertilized egg in a dish to bring about fertilization, and eventually, the development of an embryo. The embryo is ultimately transferred into the woman’s uterus. IVF as a form of treatment isn’t a one-time procedure but a carefully conducted process that may require 28 days (or more) and that it requires a series of steps and measures.
Why go for IVF?
In vitro fertilization (IVF) is one of several assisted reproductive techniques (ART) performed to treat infertility, and assist infertile couples to have a child.
According to the American Society of Reproductive Medicine (ASRM), “Infertility is a disease historically defined by the failure to achieve a successful pregnancy after 12 months or more of regular, unprotected sexual intercourse or due to an impairment of a person’s capacity to reproduce either as an individual or with her/ his partner”. Infertility as a condition is multi-factorial. Some notable explanations for infertility may be attributed to the following:
- Anatomical abnormalities like damaged or blocked fallopian tubes in females
- The hormone imbalance that may contribute to ovulation disorders that could lead to fewer eggs available for fertilization.
- Medical conditions like endometriosis in the woman, and low sperm count in men.
- History of tubal sterilization or ligation (a procedure in which the fallopian tubes are cut or blocked to permanently prevent pregnancy)
- Presence of benign tumors (in the form of fibroids) in the uterine wall which is common among women in their 30s and 40s.
- A case of mysterious infertility meaning no cause of infertility has been established despite the assessment of common causes.
- A genetic disorder is suspected hence preimplantation genetic testing, a technique that involves IVF is called for. This involves screening the eggs for certain genetic problems.
- Fertility protection in cases of cancer or other health conditions. Cancer management like radiation or chemotherapy could affect one’s fertility; hence IVF for fertility preservation may be an option. The harvested eggs are subjected to cryopreservation (or freezing) in an unfertilized state for later use.
- Women without a functional uterus and or women with delicate pregnancy posing serious health risks may choose IVF through a gestational carrier. This means that after the woman\s eggs are fertilized with sperm, the formed embryos are eventually placed in the gestational carrier\s uterus.
Preparation: Precautions and Screening Procedures
A handful of screening tests are conducted before starting an IVF cycle. The tests range from imaging studies like a transvaginal ultrasound of the female reproductive system organs (ovaries and uterus) to various blood tests to measure hormone levels.
Essential tests that are conducted include the following:
-
Ovarian reserve testing.
The term “ovarian reserve” pertains to a woman\s remaining egg supply that can produce babies. This supply is often reduced as the woman gets older. The primary tests for ovarian reserve include determining the level of follicle-stimulating hormone (FSH), anti-Mullerian hormone (AMH), estradiol, and an ovarian antral follicle in the woman’s system.
-
Semen analysis or spermiogram.
A test that evaluates certain characteristics of a male\s semen and the sperm contained therein. It is done to help evaluate male fertility, especially for those seeking pregnancy.
-
Infectious disease testing and immunity screening.
Done through a simple blood test. This testing is not directly related to fertility or the ability to conceive but helps to ensure a safe pregnancy and a healthy baby.
-
Practice or trial embryo transfer.
It is a procedure usually performed in the month before the actual IVF cycle, intending to evaluate the passage of a transfer catheter into the uterus, as well as to establish the length of the cavity, from the external cervical os to the uterine fundus.
-
Pelvic exam (primarily focused on the uterus)
This involves examining the inside lining of the uterus before the start of IVF. The evaluation may involve the following procedures:
-
sonohysterography (process wherein fluid is injected through the cervix into your uterus)
-
ultrasound scan (to generate images of the uterine cavity)
-
hysteroscopy (a process wherein a thin, flexible, lighted telescope is inserted through the vagina and cervix into the uterus).
After careful evaluation and the woman is assessed to be a qualified patient for in vitro fertilization, she will be given "fertility drugs" as part of the preparation phase or stimulation phase of the IVF plan. These medications are intended to stimulate ovulation and eventually lead to the development of multiple eggs. Examples of these drugs may include gonadotropin-releasing hormone agonists (GnRHa), follicle-stimulating hormone (FSH), a luteinizing hormone (LH), or a combination of both, and human chorionic gonadotropin (hCG) containing pills or even injections.
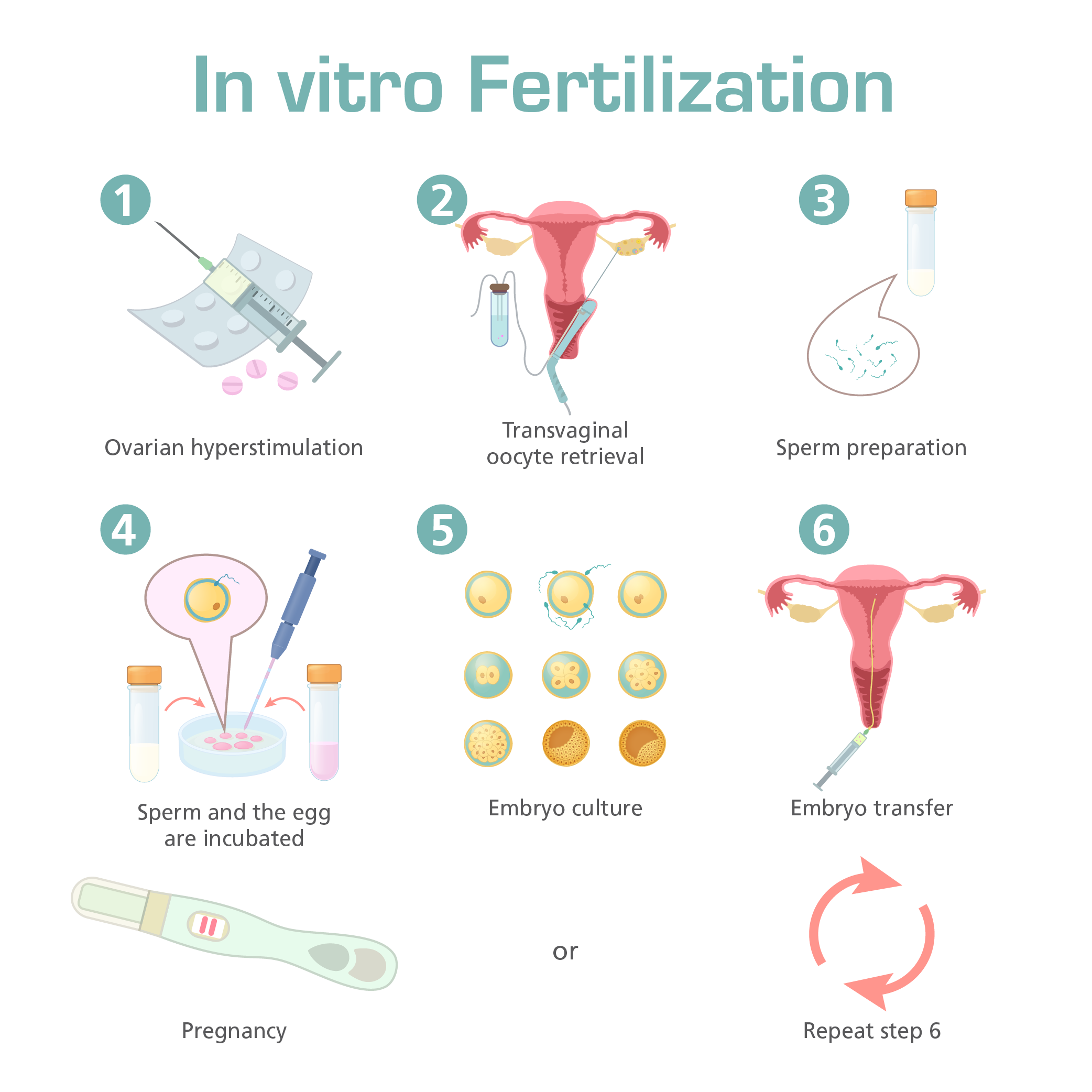
The IVF Process
The ASRM Publications describes In vitro fertilization (IVF) as a method of assisted reproduction that involves combining an egg with sperm in a laboratory dish. If the egg fertilizes and begins cell division, the resulting embryo is transferred into the woman’s uterus where it will hopefully implant in the uterine lining and further develop.
After the various screening tests are conducted, and the woman has started the stimulation phase, here is a rundown of the next crucial steps. This shows how IVF (in vitro fertilization) generally works.
Egg Retrieval
The egg retrieval or collection procedure is performed approximately 34 to 36 hours after the human chorionic gonadotropin (hCG) injection is administered. The procedure is performed under the guidance of an ultrasound, as the medical professional inserts a needle through the vagina into the woman\s ovary so that the fluid that contains mature eggs from the follicles are aspirated. The fluid removed is examined in the laboratory to verify the presence of egg cells. General anesthesia is not necessary but the woman may be sedated. This procedure generally takes around 20 to 30 minutes and is completed on an outpatient basis.
Sperm Retrieval
Concurrently, the man is asked to provide a semen sample (usually by masturbation) wherein the sperm cells are separated from the semen in the laboratory. Another method that may be done is testicular aspiration (requires the use of a needle to extract sperm directly from the testicle).
Actual Fertilization
The active sperm are then pooled in the culture dish with the ova/egg cells. This signals the actual process of in vitro fertilization. Approximately 18 hours after this procedure, the egg/ eggs have been likely fertilized and have begun to divide into embryos. The use of an incubator comes into play wherein the fertilized eggs are cultivated under controlled conditions until they reach the blastocyst stage (usually day 5 in the laboratory).
Embryo Transfer
Any day between days 17 to 19 (depending upon the maturation of the embryos), the fertilized embryos are transferred into the uterine cavity. To ascertain that the embryos are transferred into the correct place, another ultrasound scan is performed.
The number of embryos for transfer is a joint decision jointly by the medical professional and the woman herself. The recommendation and decision to be made depending on certain factors like a woman\s age, her reproductive history, the risk of multiple pregnancies, and the excellence and appearance of the fertilized embryos.
The procedure involves the transfer of the embryos into the woman\s uterus through the cervix using a catheter, and a speculum like a uterine exam. Just like the retrieval process, anesthesia is not required.
Luteal Phase of the Cycle
After the embryo transfer, the woman is given the hormonal drug that contains injectable or vaginal progesterone that will go on for 2 weeks. After this, a pregnancy test is scheduled to know if the implantation is successful.
So how long does an IVF (in vitro fertilization) process take place? Here is a sample 28-day IVF Plan that will give you a quick look as to how the process happens.
A 28-day IVF Plan in a Nutshell
|
Day 1
|
Day 2
|
Day 3
|
Day 4
|
Day 5
|
Day 6
|
Day 7
|
|
1st day of a woman’s period
|
Stimulation Phase: Treatment begins with medications within the first 2-3 days of a woman’s period. Examples of medications include fertility tablets and or injections that contain Follicle Stimulating Hormone - FSH. One may also take medicine that inhibits normal pituitary function in order to prevent ovulation prior to egg collection.
|
|
Day 8
|
Day 9
|
Day 10
|
Day 11
|
Day 12
|
Day 13
|
Day 14
|
|
The day when the monitoring of IVF treatment cycle through various blood tests and ultrasound scans begin.
|
|
Another round of ultra sound scan is conducted as a means of closely monitoring the follicular development and reaction/s to the medication given.
|
|
Schedule of a third scan. Once the ova/eggs are ready for collection, a trigger injection will be given in the evening. That drug is a Human Chorionic Gonadotropin – HCG) containing injection.
|
|
Egg retrieval/ collection.
A transvaginal ultrasound is conducted, and the eggs are extracted using a fine needle attached to the ultrasound.
Also, the follicular fluid is checked under a microscope to know how many eggs were collected.
Progesterone-containing medication is given after the eggs are collected to prepare the lining of the womb for embryo transfer.
Sperm retrieval. At the same day, a fresh sample of sperm is collected to initiate fertilization in the laboratory after collection processes.
|
|
Day 15
|
Day 16
|
Day 17
|
Day 18
|
Day 19
|
Day 20
|
Day 21
|
|
Fertilization. In the next 3 – 5 days, the embryos or the fertilized eggs are cultivated under controlled conditions inside the laboratory, until they reach the blastocyst stage (usually day 5 in the laboratory).
Depending on what happens during the process, any day between days 17 to 19, the fertilized embryos are transferred into the uterine cavity (fresh embryo transfer process).
In order to ascertain that the embryos are transferred into the correct place, another ultrasound scan is performed.
|
Luteal Phase of the Cycle.
After the process of embryo transfer, several medications will be given to the patient. These include the following: progesterone, folic acid tablets and sometimes aspirin or heparin injections would be prescribed.
|
|
Day 22
|
Day 23
|
Day 24
|
Day 25
|
Day 26
|
Day 27
|
Day 28
|
|
|
|
|
|
|
|
Pregnancy Test. Last step is the performance of a pregnancy test via β-hCG. This will determine if implantation is successful.
|
Risks and Results
Risks of Undergoing IVF
Like most invasive procedures, IVF also has certain risks. Specifically, egg retrieval procedure complications can occur that are manifested in the form of bleeding, damage to the bowel (and/ or near-by organs), and infection. During the stimulation phase, the use of certain medications can cause ovarian hyperstimulation syndrome (OHSS) wherein a woman may experience bloating, cramping sensation, and an increase in weight. Also, the probability of a “cancelled cycle” may occur in cases wherein a woman does not respond satisfactorily to the stimulation medications, and when an inadequate number of follicles is produced. Noteworthy to mention is the stress IVF can cause financially, physically, and emotionally. Hence, the support from family, friends, and health care professionals throughout the infertility treatment journey, is very essential.
Results: The Good and the Bad
The success rate of IVF usually varies among clinics and medical professionals conducting the procedure; hence, pregnancy is not guaranteed. In most instances, the process may have to be done more than once to achieve gestation. According to studies, IVF success rates have improved over the years.
On the other end of the spectrum, a case of ectopic or multiple pregnancies may lead to spontaneous abortion or termination of pregnancy if the woman’s health is deemed at risk.
Other Assisted Reproduction Techniques (ART)
IVF is just one method that could treat infertile patients. Other Assisted Reproduction Techniques (ART) that have been used as alternatives to IVF are the following:
-
Gamete Intrafallopian Transfer
A procedure similar to IVF, GIFT is used when a woman has at least one normal fallopian tube. The egg cells are positioned in this tube together with the man\s sperm for fertilization to occur.
-
Zygote intrafallopian Transfer (ZIFT)
This transfer technique refers to a procedure in which a woman\s oocytes are taken from her ovaries, undergoes fertilization in the laboratory, and eventually inserted into her fallopian tubes instead of the uterus.
-
Embryo cryopreservation (fertilized egg and sperm freezing)
If more embryos have developed (than transferred to the woman\s uterus), the embryos can be transferred or used during a future cycle.
-
Intracytoplasmic Sperm Injection (ICSI)
This is a manipulation technique that requires the use of a microscope to inject a single sperm into the egg cells before the fertilized eggs are transferred into the woman\s body.
Esco Medical’s Line of IVF Incubators and Workstations
The whole IVF process is very delicate and needs to ensure optimum environmental conditions for the embryos. To ensure this, Esco Medical has produced a product line specially designed to safeguard the developing embryos.
Embryo handling has never been this efficient with Esco Medical’s Multi-Zone ART Workstations (MAW). These workstations guarantee optimum temperature conditions with its multi-zone heating elements even outside the incubators. Esco Medical also boasts of a line of incubators ideal for the growth of a developing embryo.

Our range of MIRI® Multiroom incubators ensures that there is no disturbance whenever there is embryo handling on neighboring chambers. After opening and closing chambers, our incubators possesses quick temperature recovery times of <1 minute and <3 minutes for gas recovery.
Esco Medical’s MIRI® Time-Lapse Incubator enables zero disturbances to the embryo all while giving the Embryologist to observe the whole development of the embryos. This feature gives them enough information on what embryos to select for transfer and in turn shortening the time to achieve pregnancy.
For more information about these innovative, world-class IVF solutions, visit Esco Medical’s product page at https://www.esco-medical.com/





